A patient is receiving mechanical ventilation by the septic shock, which he developed due to Fournier´s perineal gangrene. One day after surgical revision of the necrosis, laparoscopy with cholecystectomy and establishment of double-barrelled ileostomy was performed (to prevent contamination of perineum by spontaneous defecation).
Patient´s history encompasses hypertension, chronic ischemic heart disease, state after myocardial infarction of inferior wall with implantation of stent ten years ago, dual-chamber stimulation, chronic heart failure, NYHA III, permanent atrial fibrillation, diabetes mellitus II.
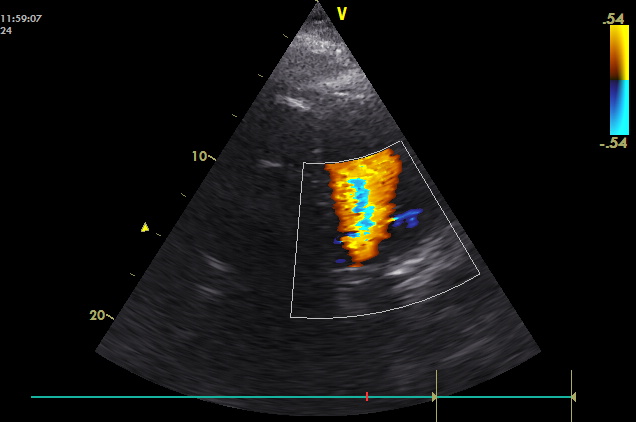
Patient in weaning protocol (CPAP with PEEP 8, FiO2 0.4), gradual decreasing of the noradrenalin dose (1 mg/hour, i.e. approximately 0.15 ug/kg/min at the moment), mean arterial pressure was kept around 70 mmHg, stable heart rate of 60 bpm maintained by the pacemaker. Periphery was colder, capillary refill time 4 s, the normal value of lactate, anuria, CVVHD, negative fluid balance.
Is actual perfusion sufficient? Will there be any benefit after administration of fluid or inotropic agents?
Echocardiography was performed:
<h3>